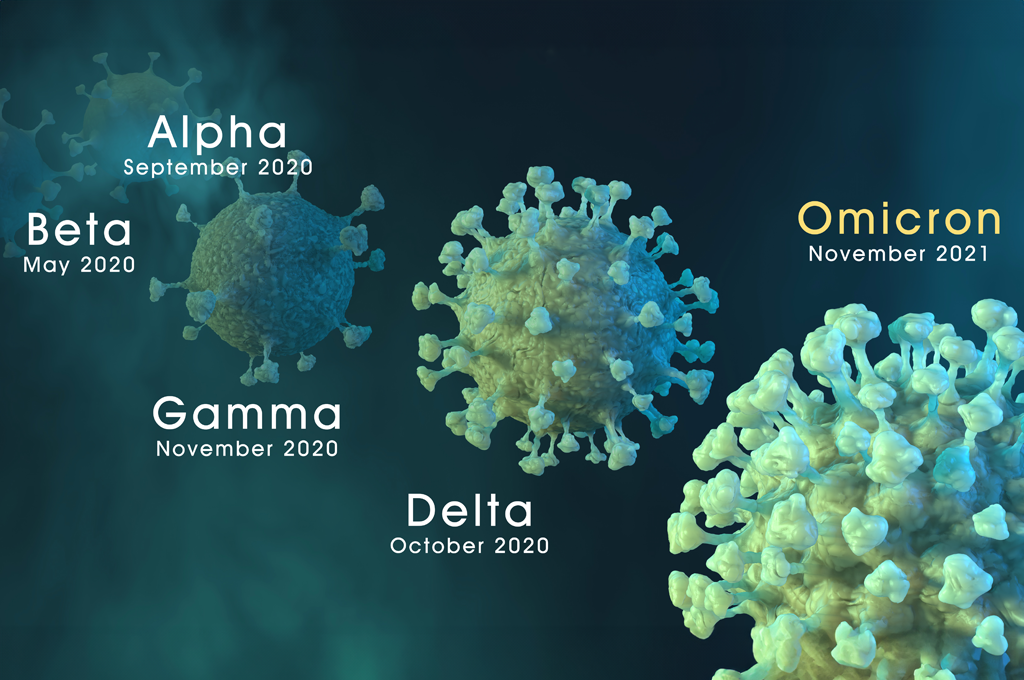
As summer days turn to fall, we embark once again on the annual flu and RSV season. However, this rise in viruses also includes various mutations of SARS-CoV-2, the virus that causes COVID-19. The WHO is currently monitoring three variants which first appeared in 2023: Pirola (BA.2.86), Eris (EG.5), and Arcturus (XBB.1.16). All three are descendants of the Omicron strain.
Pirola (BA.2.86)
Appearing in Denmark in late July, Pirola has an unexpected lineage. Per the Global Center for Health Security, Pirola “seems to have come from the older BA.2 omicron lineage that was dominant in early 2022 and not from the newer omicron offshoots.”
“The new lineage has more than 30 mutations on its spike protein, which helps the virus latch onto cells and cause infection,” says The Washington Post. “That could make it better at evading immunity from vaccines and past infections.” The infected may expect symptoms similar to Omicron: fever, continuous cough, runny nose, aches and pains, changes in taste and smell, and tiredness. Pirola may be more likely to cause diarrhea than other Omicron strains. As of September, there is no concrete evidence that indicates the Pirola subvariant causes more severe illnesses.
Eris (EG.5)
Appearing in February 2023, EG.5 has seen exponential growth. As cited by the Washington Post, “EG.5 made up an estimated 17.4% of global cases in the week ending July 23 […] up from only 7.6% four weeks earlier.”
Unlike Pirola, Eris evolved from the XXB strains of Omicron. What sets the Eris apart from its parent lineages is a particular mutation in its spike protein — F456L. The CDC considers all viruses containing this mutation (including Eris) to be “variants of interest.”
According to the Irish Star, a unique symptom of Eris may include night sweats. More typical Omicron symptoms include, “sore throat, runny nose, blocked nose, sneezing, dry cough, headache, wet cough, hoarse voice, muscle aches, [and] altered smell.” However, “symptoms that once were common — such as the loss of smell and taste — are becoming less common with Omicron variants.”
Arcturus (XBB.1.16)
Like Eris, Arcturus evolved from XBB subvariants. According to a letter to the editor submitted to the Journal of Taibah University Medical Sciences, “The XBB.1.16 subvariant has a proliferative edge and can evade the immune system. It has been spreading rapidly on a global scale and has been linked with a higher effective reproductive number than other subvariants.” (Note that some popular sources refer to Arcturus as subvariant XBB.1.18., but this appears to be an error.)
Per a feature in The BMJ, Arcturus is “present in at least 33 countries[…;]at one point in April India was seeing 10 000 confirmed cases a day—nearly two thirds of all covid-19 in the country, and necessitating the return of mask mandates. Case numbers are now receding [sic].” However, that doesn’t mean the United States is out of the woods. In August, Today reported that Eris and Arcturus “are now the most prevalent COVID-19 [variants] worldwide, both accounting for 21% of sequences globally.”
Per the WHO, “The global risk assessment for XBB.1.16 is comparable to the other currently co-circulating XBB variants[…]no changes in severity have been reported in countries where XBB.1.16 is reported to be circulating.”
Ensuring Best Practices
According to the aforementioned article in Today, “During the last two weeks, there was a 20.2% increase in the number of average daily COVID-19 hospitalizations.” While the raw numbers are nowhere near the rate of hospitalization experienced during the height of the pandemic, any hospitalizations may be considered a failure of earlier precautionary measures. This is especially relevant for people who are older, have multiple comorbidities, or are immunocompromised. We have tools to limit infections, and we ought to use them.
As individuals, it’s now more important than ever to test (after exposure or at the onset of symptoms), especially as RSV and the flu — which share similar symptoms with COVID-19 — begin to emerge. This will allow you to avoid situations where you can infect others, and to obtain treatment if needed. The CDC also offers a series of tools for determining when you may wish to mask.
Organizations should look to the pioneers of clean air policy. Clean indoor air is more important than ever as the cool, winter weather forces us inside. Proper ventilation, air cleaning, and filtration are key to reducing the transmission of viruses.
To ensure that your space receives layered protection against harmful pathogens — including the virus that causes COVID-19 — equip your home or building with air purification technology that provides real-world results. Devices with ActivePure® Technology have been proven to reduce up to 99.9% of SARS-CoV-2 both on surfaces and in the air, but that’s not all. We’ve also been tested in the field. View ActivePure’s peer-reviewed testing results to learn how our devices perform in a busy COVID ward.